February 16, 2021
By Matt Dionne
Diversity is now rightly a corporate priority in America. Companies large and small know that improving their diversity and inclusion policies will improve their culture and workforce. And Pharma is no different. Pharmas want more diverse representation in management, their boards, and in clinical trials. Should a similar lens be applied to access and reimbursement challenges – and in particular to patient support programs?
Real Endpoints (RE) surveyed 209 patients with specialty diseases to determine whether patients from underrepresented groups faced patient support challenges majority groups did not.
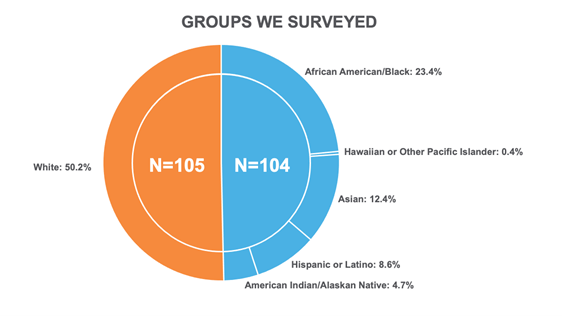
There was plenty of good news. Once a patient gets to the manufacturer’s patient support program there is very little difference in the experience. Majority and underrepresented groups both reported positive interactions. All are being treated with compassion and are satisfied with turn-around times.
However, we found crucial discrepancies between groups in their journey to the patient support program, in three areas in particular. Cost and affordability is something many patients believe is a factor prior to treatment decision, but it’s not always part of the conversation.
Patients are also not consistently receiving the manufacturer’s educational materials on financial assistance. Lastly, patients are not reaching out to the hub unless someone educates them about it, and even then, there are discrepancies.
Unseen Barriers to Entry
With drug pricing constantly in the news, it’s no surprise that some patients believe cost to be an important factor in their prescribers’ final prescription recommendations. But underrepresented groups thought cost was even more important.
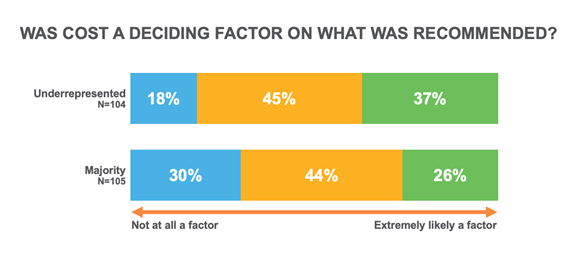
Underrepresented men were particularly sensitive on this point – as if cost was the deciding factor. In essence they believe they’re being steered to lower-cost and perhaps less effective options. It is critical that manufacturers do more to raise awareness of the financial assistance options that should make cost a nonissue. The focus should be on clinical efficacy, not price.
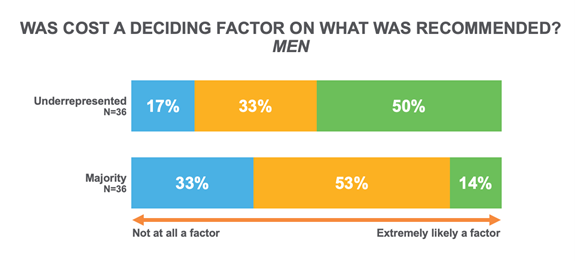
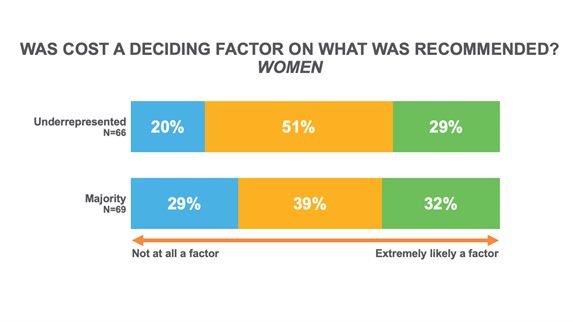
While cost is sometimes discussed between patients and their providers, our data shows that providers aren’t helping close the gap. Patients from underrepresented groups were less likely to be approached by their doctor about the cost of treatment. The problem was particularly acute in urban settings. Doctors initiated discussions on treatment costs with only half of the patients from underrepresented groups, as opposed to the two-thirds of patients from the majority group.
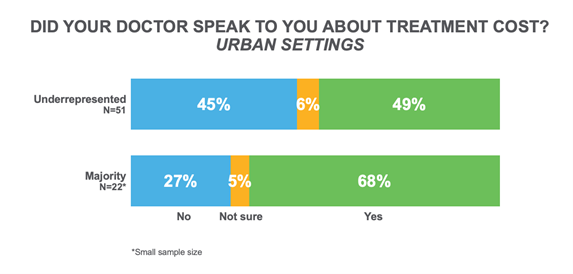
The situation is exacerbated by the fact that discussing treatment costs with patients is an informal process. According to diversity and inclusion research, underrepresented groups are less likely to be familiar with such informal processes ahead of time. Therefore, manufacturers need to provide as much documentation for these processes as possible.
Patient Materials: Often a Wasted Effort
A great deal of time and money is spent creating and disseminating materials for patients in order to educate them on financial resources available through the manufacturer’s patient support program. In general, they’re quite good – understandable and helpful from the point of view of underrepresented and majority groups. Most patients (94% overall) noted that the materials they did receive were in their preferred language. Patients found it easy to understand the educational materials on financial assistance, and there was no significant difference between groups.
Unfortunately, a lot of the effort spent on this material is wasted. Majority group patients reported receiving financial education materials less than half of the time. Underrepresented groups lag even further behind: 2 out of 5 underrepresented patients reported that they received this material.
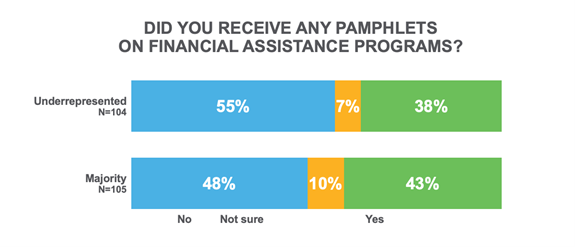
Trusted Sources Patients Rely On
The importance of these educational materials is indeed significant. Patients are much more likely to reach out to the patient support program if they have received educational materials. Again, we found underrepresented groups were left behind, as they are less likely to reach out to the manufacturer hub for help.
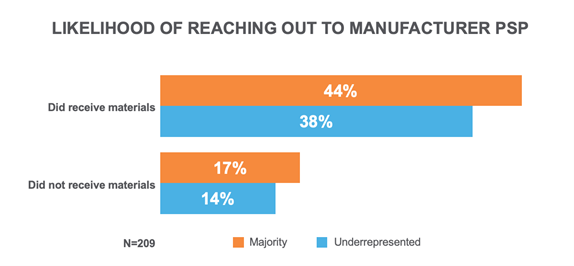
Small Steps Forward
Our findings show that patients in underrepresented groups are less likely to be informed about cost, receive educational materials, and reach out to the manufacturer patient support program. So, what can be done about it? First, we need to capture race on enrollment forms and then use the data to improve our patient support programs. In a review of the top 10 patient support service programs’ applications, none of them captured race. One common response from our clients when we make this recommendation is that “we only capture information relevant to reimbursement and access, and race does not help us determine a patient’s coverage”.
But that’s nonsense. Gender is equally irrelevant to determining a patient’s coverage, yet all programs capture this detail. For companies who want to make a program effective for all patients, they’ll need to start capturing this information. There is no way to start measuring a patient support program’s effectiveness at helping or reaching underrepresented groups if this information is not captured for each patient. Once a hub starts capturing it they can make informed decisions about moving away from a “one-size fits all” approach to educational materials, and do more to explain processes and steps along the way that patients may be unaware of. Above all, more companies need to focus on getting these materials into the hands of patients that require support. Adding diversity as a measurement will begin real steps towards the mission of improving access for all patients.
Note: The stacked bars charts represent Likert scale questions with answers rated from 1 to 7.
For more information on the demographic breakdown cuts of this survey
or, if you would like to see more survey results, please contact info@realendpoints.com.
